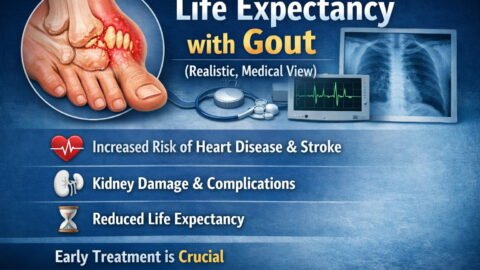
Uric acid is a natural waste product formed when your body breaks down purines. Purines are found in your own cells and also in many foods. Most of the time, uric acid dissolves in the blood, travels to the kidneys, and leaves the body through urine. When production rises too high or removal becomes inefficient, uric acid builds up in the bloodstream. This state is commonly called high uric acid or hyperuricemia.
High uric acid does not always cause symptoms, but it raises the likelihood of urate crystals forming in joints and tissues. Those needle like crystals can trigger gout, a painful inflammatory arthritis that often strikes suddenly.
What Uric Acid Does in the Body
Uric acid is the end point of purine metabolism. Your body continuously recycles DNA and other cell components, so purine breakdown happens every day. A smaller portion comes from dietary purines.
Uric acid itself is not automatically harmful. In fact, it has antioxidant properties in the bloodstream. The problem arises when the balance between production and excretion is disturbed for long enough that urate becomes overly concentrated.
Normal Uric Acid Range
Laboratories may use slightly different reference ranges, and results can vary depending on hydration, recent diet, alcohol intake, and certain medications. Still, typical adult ranges often fall into the following patterns.
Table 1: Common Serum Uric Acid Ranges in Adults
| Group | Typical Range in mg per dL | Notes |
|---|---|---|
| Adult men | 3.4 to 7.0 | Upper levels are more common due to hormonal and metabolic factors |
| Adult women | 2.4 to 6.0 | Levels may rise after menopause |
| Children and adolescents | 2.0 to 5.5 | Range depends on age and growth stage |
A result slightly above the reference range does not automatically mean gout. Risk depends on the level, the duration, genetics, kidney function, body weight, diet patterns, and other medical conditions.
When Uric Acid Becomes “High”
Hyperuricemia generally refers to serum uric acid above the lab upper limit. Clinically, the risk of crystal formation rises as levels increase and stay elevated.
Table 2: How Elevated Uric Acid Relates to Risk
| Serum uric acid in mg per dL | What it often means | Typical risk trend |
|---|---|---|
| Under 6.0 | Often considered favorable for people with gout history | Lower chance of urate crystal formation |
| 6.0 to 6.9 | Borderline high in many labs | Risk can rise in susceptible people |
| 7.0 to 8.9 | Clearly elevated for most adults | Higher probability of urate crystal buildup over time |
| 9.0 and above | Markedly high | Substantially higher risk of gout flares and kidney related urate issues |
For people who already have gout, clinicians often aim for a lower uric acid target over time because keeping urate lower helps dissolve existing crystals gradually and reduces flare frequency.
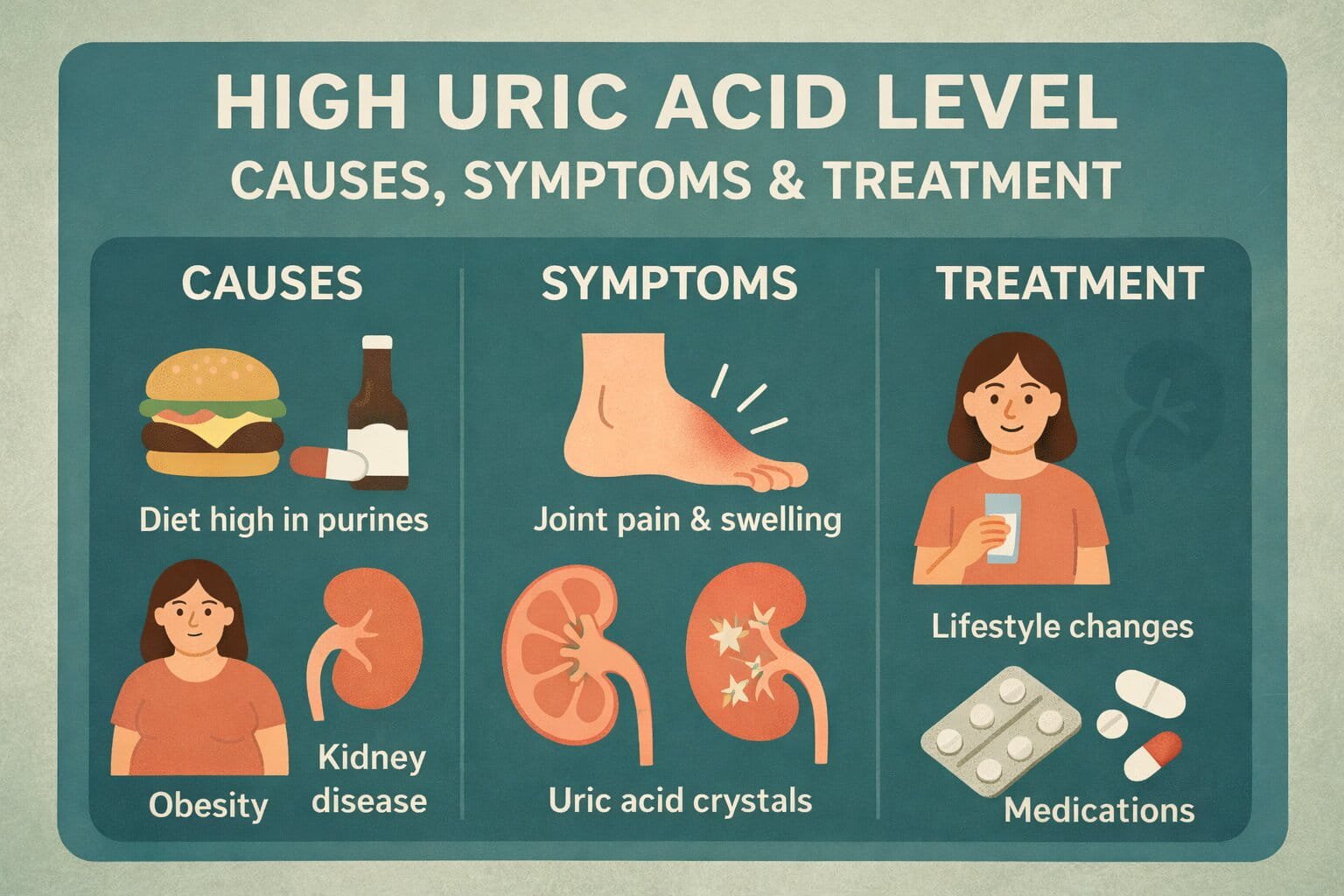
Why Uric Acid Goes Up
High uric acid usually happens for one of two reasons, sometimes both. Your body makes too much, or your kidneys do not remove enough.
1) Reduced excretion through the kidneys
This is one of the most common reasons. Kidney function does not need to be severely impaired for urate clearance to decline. Mild reduction can still raise levels.
2) Increased production of uric acid
This can occur with high purine intake, increased cell turnover, or certain metabolic states.
Table 3: Common Factors That Raise Uric Acid
| Category | Examples | How it contributes |
|---|---|---|
| Diet patterns | Organ meats, certain red meats, anchovies, sardines, some shellfish | Higher purine load increases urate production |
| Drinks | Alcohol, especially beer and spirits, sugary drinks with fructose | Alcohol reduces excretion, fructose increases production |
| Body weight and metabolism | Overweight, insulin resistance, metabolic syndrome | Impairs urate clearance and increases inflammation |
| Kidney related factors | Chronic kidney disease, dehydration | Less urate removal through urine |
| Medications | Certain diuretics, some low dose aspirin, specific immunosuppressants | Can reduce urate excretion |
| Rapid cell turnover | Psoriasis flares, some cancers, chemotherapy, hemolysis | More purine breakdown raises uric acid |
| Genetics | Family history of gout or hyperuricemia | Affects transporters involved in urate handling |
Not everyone with these factors develops gout, but the combination of elevated urate and susceptibility increases the odds.
High Uric Acid vs Gout: What’s the Difference?
High uric acid is a lab finding. Gout is a clinical condition caused by immune reaction to monosodium urate crystals. Many people have hyperuricemia without gout, and a smaller group can have gout even if their uric acid is not very high at the moment of a flare. During a sudden attack, urate levels can temporarily dip because crystals are moving from blood into joints.
So, a single blood test never tells the whole story. Trend over time, symptoms, and clinical evaluation matter.
How Gout Develops and Why It Hurts So Much
When urate is high for long enough, crystals can form in cooler areas of the body such as the big toe joint. A flare often begins at night and builds quickly. The immune system treats crystals like a threat and releases inflammatory signals. This causes intense pain, swelling, warmth, redness, and tenderness. Even a bedsheet touching the joint can feel unbearable.
Over years, repeated crystal deposition can lead to:
Joint damage and reduced mobility
Tophi, which are firm urate deposits under the skin
Frequent flares that become harder to predict
Kidney stones or kidney stress in some individuals
Symptoms That Suggest High Uric Acid Might Be Becoming a Problem
High uric acid itself is often silent. But certain patterns should raise concern:
Sudden severe joint pain, commonly in the big toe, ankle, knee, or midfoot
Swelling and redness in one joint that peaks within hours
Recurrent attacks with symptom free intervals
A history of kidney stones or gritty urine discomfort
Firm lumps near joints, ears, fingers, or elbows
If these symptoms appear, it is wise to discuss testing and management rather than waiting for repeated flares.
Testing Uric Acid: What to Know
A simple blood test measures serum uric acid. For gout evaluation, clinicians may also consider:
Inflammation markers and kidney function tests
Urinalysis and urine uric acid in selected cases
Joint fluid analysis to confirm urate crystals when diagnosis is uncertain
Imaging such as ultrasound or dual energy CT in specific situations
Testing works best when interpreted alongside symptoms and medical history. If you had a recent flare, your clinician may repeat levels later to understand your baseline.
Lowering Uric Acid Naturally Through Lifestyle
Lifestyle changes can meaningfully reduce uric acid and also improve overall metabolic health. They are especially helpful for people with borderline high levels or early gout, and they support medication effectiveness for those who need it.
Hydration
Drinking enough water helps the kidneys flush urate. Dehydration concentrates uric acid and can encourage crystal formation.
Weight management
Gradual weight loss can lower urate and reduce inflammation. Crash diets and fasting can backfire because rapid ketosis may raise uric acid temporarily.
Smarter carbohydrate choices
Reducing sugary drinks and excess fructose is often more impactful than many people realize. Fructose can stimulate urate production and worsen insulin resistance.
Alcohol moderation
Beer and spirits tend to increase gout flare risk more than other options. Alcohol also interferes with urate excretion.
Protein choices that reduce flare risk
You do not need to remove all protein. Many people do well with:
Low fat dairy
Eggs
Plant proteins such as lentils and beans in moderate portions
Lean poultry or fish choices selected carefully
Triggers vary by individual, so patterns over time matter.
Table 4: Practical Food and Drink Guidance
| Prefer more often | Limit or reduce | Why it helps |
|---|---|---|
| Water, unsweetened tea, coffee in moderation | Sugary sodas, sweet juices, energy drinks | Lower fructose load supports urate control |
| Low fat milk, yogurt | Heavy cream and high sugar dairy desserts | Dairy may support urate clearance when low in sugar |
| Fruits in whole form | Large amounts of fruit juice | Whole fruit has fiber, juice spikes sugar load quickly |
| Vegetables, whole grains | Refined carbs and frequent sweets | Better insulin sensitivity can improve urate handling |
| Lean proteins in balanced portions | Organ meats and frequent large red meat portions | High purine density can raise urate production |
| Balanced meals | Crash dieting and prolonged fasting | Rapid metabolic shifts can raise uric acid |
If you already have gout, individualized trigger tracking can help. A flare diary that notes foods, alcohol, sleep, dehydration, stress, and activity can reveal your strongest patterns.
Medical Management Options
Lifestyle changes may be enough for some people, but others need medication. Treatment depends on symptoms, uric acid level, flare frequency, presence of tophi, kidney function, and other health conditions.
Medications used during a flare
These help calm inflammation and pain. They do not dissolve urate crystals immediately, but they reduce the attack intensity and duration when started early.
Long term urate lowering therapy
For recurrent gout, tophi, or very high uric acid, clinicians may recommend long term urate lowering therapy to reduce crystal burden over time. The goal is to keep urate consistently lower so crystals gradually dissolve and flares become less frequent.
Never start or stop prescriptions on your own. If you suspect gout, proper diagnosis is important because several conditions can mimic gout, including joint infection and pseudogout.
Who Is at Higher Risk of Gout
Gout risk rises with:
Male sex and increasing age
Menopause and postmenopausal hormonal changes
Family history of gout
Obesity, insulin resistance, and type 2 diabetes
High blood pressure and certain cardiovascular risks
Chronic kidney disease
Regular alcohol intake
High intake of sugary drinks
Use of certain diuretics
FAQs
1) What is a normal uric acid level?
Normal varies by lab, but many adult men fall around 3.4 to 7.0 mg per dL and many adult women around 2.4 to 6.0 mg per dL. Your report range is the best reference for your test.
2) Can you have high uric acid without gout?
Yes. Many people have hyperuricemia with no symptoms. Gout happens when urate crystals form and trigger inflammation, which does not occur in everyone with elevated levels.
3) What uric acid level is strongly linked to gout attacks?
Risk rises as levels go higher and stay high. Levels around 9.0 mg per dL or above are often associated with a much higher chance of crystal buildup and gout flares over time, especially with other risk factors.
4) Why does gout often start in the big toe?
The big toe joint is cooler and experiences frequent micro stress during walking. Urate crystals form more easily in cooler areas, making the big toe a common first site.
5) Does drinking a lot of water lower uric acid?
Good hydration supports kidney clearance of urate and may reduce the chance of crystals forming. It can help, but it may not be enough alone if uric acid is very high or if gout is recurrent.
6) Are all high purine foods equally risky?
No. Individual response varies, and food context matters. Organ meats and certain seafood are common triggers. Many people tolerate moderate portions of other proteins, especially when overall diet quality is good.
7) Is fruit bad for gout because it has fructose?
Whole fruit in normal portions is usually fine for most people because fiber slows absorption. The bigger issue is sugary drinks and large amounts of fruit juice, which can deliver concentrated fructose quickly.
8) Can uric acid be normal during a gout flare?
Yes. During an acute flare, blood uric acid can fall temporarily. If gout is suspected, repeat testing later and consider crystal confirmation when needed.
9) How fast can uric acid levels improve with lifestyle changes?
Some improvement can happen within weeks, especially with less sugary drinks, less alcohol, better hydration, and gradual weight loss. Larger changes and stability often take longer because metabolism and kidney handling adapt over time.
10) When should someone consider long term urate lowering therapy?
It is often considered for recurrent flares, tophi, joint damage, very high uric acid, or kidney stone history. A clinician decides based on your overall risk profile, kidney function, and flare pattern.
Key Takeaway
Uric acid is normal and unavoidable, but consistently high levels increase the chance of urate crystal formation. That is what raises gout risk, especially when combined with kidney clearance issues, metabolic factors, and certain dietary patterns. If you have repeated joint attacks, a history of kidney stones, or very high readings, a structured plan that combines lifestyle changes with appropriate medical care can dramatically reduce flares and protect long term joint health.